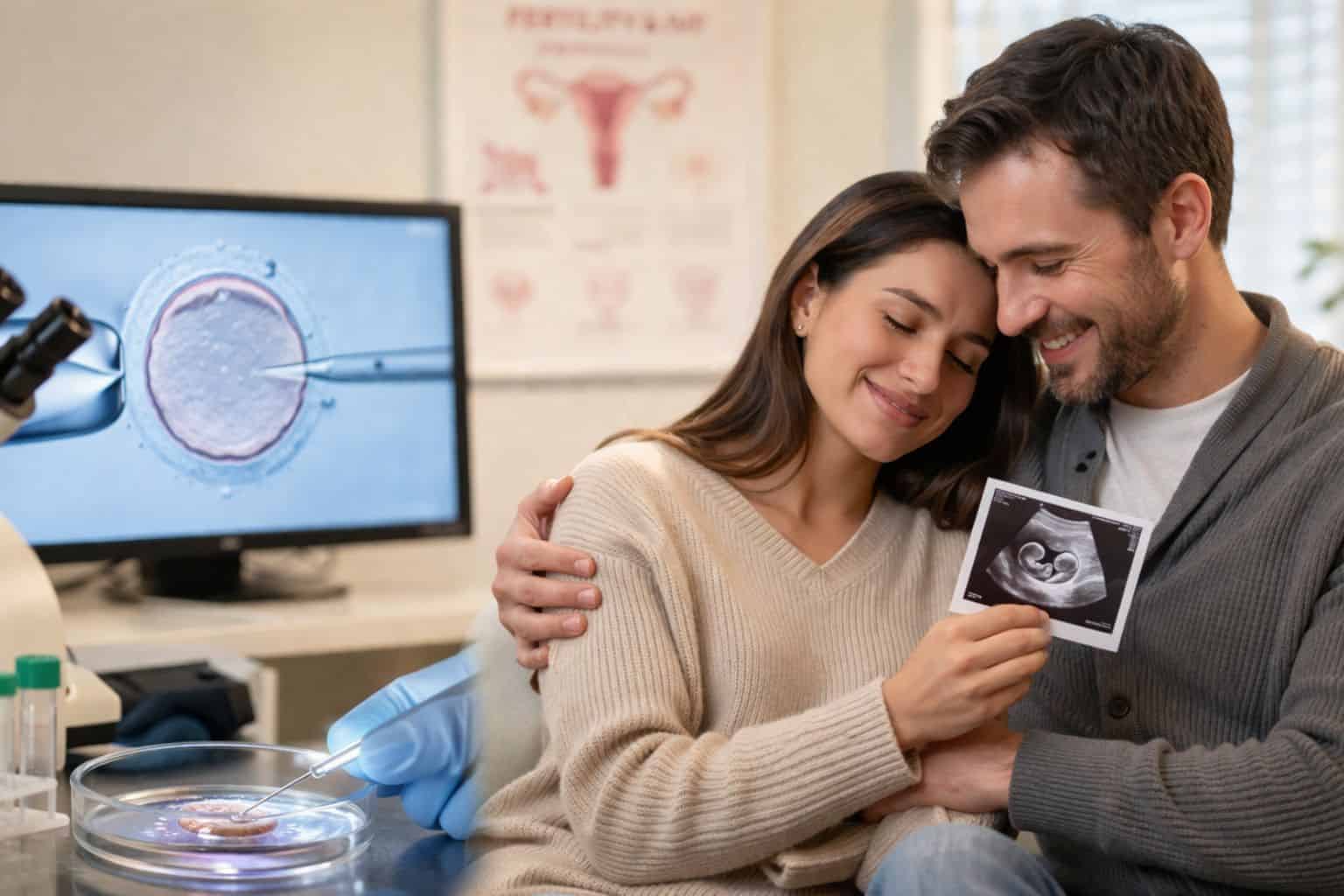
IVF (In Vitro Fertilization) is a medical fertility treatment in which a woman’s eggs are retrieved from her ovaries, fertilized with sperm in a laboratory, and the resulting embryo is transferred into the uterus to establish a pregnancy. It is the most effective form of assisted reproductive technology (ART) available today, used to treat blocked fallopian tubes, male infertility, PCOS, endometriosis, unexplained infertility, and age-related fertility decline.
In Nepal, IVF is particularly important because approximately 15 to 20% of couples of reproductive age face infertility, yet access to specialist fertility care has historically been limited and concentrated in Kathmandu. Since Nepal’s first IVF baby was born in 2005, the country has developed a growing network of clinics offering IVF at a fraction of the cost charged in India or Western countries, making treatment accessible for Nepali couples without requiring travel abroad.
What Does IVF Actually Mean?
IVF stands for In Vitro Fertilization. The phrase comes from Latin: “in vitro” means “in glass,” referring to the laboratory vessel in which fertilization takes place outside the body. The full term describes exactly what happens: an egg and sperm are combined and fertilized in a laboratory, rather than inside a woman’s body.
According to the Cleveland Clinic, IVF is a type of assisted reproductive technology (ART) in which eggs are retrieved from the ovaries and manually combined with sperm in a lab. The fertilized egg, now called an embryo, is then transferred into the uterus. Pregnancy occurs when this embryo implants itself into the uterine lining and continues to develop.
The term “test-tube baby,” which many Nepali families are more familiar with, comes from the early history of the technology. In practice, IVF does not use a test tube. It uses a petri dish in a precisely controlled laboratory environment. The science has come a long way since that naming, but the core concept remains the same: conception happens outside the body, under medical supervision, and the resulting embryo is then placed inside the uterus where a healthy pregnancy can develop naturally from that point forward.
Robert Edwards, the physiologist who co-developed IVF, was awarded the Nobel Prize in Physiology or Medicine in 2010. The first IVF baby in the world, Louise Brown, was born in England in July 1978. By 2023, an estimated 12 million children had been born worldwide through IVF and other assisted reproductive techniques.
How IVF Works: The Process Step by Step

An IVF cycle typically takes four to six weeks from the start of ovarian stimulation to the pregnancy test. It involves several distinct phases, each building on the last.
Step 1: Initial Consultation and Assessment
Before any treatment begins, both partners undergo a full evaluation. This includes hormonal blood tests for the woman, including AMH (Anti-Müllerian Hormone) and FSH to assess ovarian reserve, an ultrasound to evaluate the uterus and ovaries, and a semen analysis for the male partner. The results determine the treatment protocol, the medications needed, and the most appropriate fertilization technique (standard IVF or ICSI).
Step 2: Ovarian Stimulation
In a natural menstrual cycle, a woman produces one egg. IVF aims to retrieve multiple eggs to give the best chance of creating at least one viable embryo for transfer. The woman takes daily hormone injections, usually for 8 to 14 days, to stimulate the ovaries to mature several follicles simultaneously.
These are the same hormones the body produces naturally. The medications simply elevate them to encourage greater egg production. During this phase, the response is monitored closely through blood tests and ultrasound scans, sometimes every two to three days, so the doctor can adjust dosing and plan the timing of retrieval precisely.
Step 3: Trigger Injection and Egg Retrieval
When the follicles reach the right size, a trigger injection is given. This is timed precisely so that approximately 36 hours later, the eggs are mature and ready for collection.
Egg retrieval is a minor procedure done under light sedation. Using ultrasound guidance, a fine needle is passed through the vaginal wall into each ovary to draw out the fluid from each follicle. The embryologist in the laboratory then searches the fluid for eggs and places them in a protected incubator. Most women go home the same day with minimal discomfort.
Step 4: Sperm Collection and Fertilization
On the same day as egg retrieval, the male partner provides a semen sample. If sperm problems have been identified, frozen or surgically retrieved sperm can also be used.
Fertilization then occurs in one of two ways:
In conventional IVF, 25,000 to 50,000 prepared sperm are placed together with each mature egg in a dish, and fertilization proceeds naturally over the following hours.
In ICSI (Intracytoplasmic Sperm Injection), the embryologist selects a single healthy-looking sperm under high magnification and injects it directly into the egg. This method is used when sperm quality, count, or motility is significantly impaired, or when previous IVF cycles failed to achieve fertilization.
Approximately 18 to 24 hours later, the laboratory confirms whether fertilization has occurred. On average, 70 to 90% of mature eggs fertilize successfully during this stage.
Step 5: Embryo Culture and Development
Fertilized eggs become embryos and are monitored in the laboratory for three to five days as they divide and develop. The embryology team evaluates their quality and development rate daily. By day five or six, the healthiest embryos have reached the blastocyst stage, which has the highest implantation potential.
Any embryos not transferred can be frozen (vitrified) for future use. This means one egg retrieval can potentially support multiple transfer attempts.
Step 6: Embryo Transfer
Embryo transfer is a straightforward procedure that does not require anesthesia and takes only a few minutes. With ultrasound guidance, a thin flexible catheter is passed through the cervix, and one or two embryos are gently placed into the uterine cavity. Most women return home within an hour.
After transfer, the woman takes progesterone medication to support the uterine lining while waiting to find out whether implantation has occurred.
Step 7: Pregnancy Test
Approximately 12 to 14 days after embryo transfer, a beta hCG blood test measures the pregnancy hormone to determine whether the cycle was successful. A rising hCG level confirms pregnancy, and an ultrasound is scheduled approximately two weeks later to confirm the pregnancy is developing normally inside the uterus.
Who Needs IVF?

IVF is not the first treatment tried for every couple struggling to conceive. It is typically recommended when simpler options have not worked, or when the specific cause of infertility makes it the most effective starting point.
The conditions for which IVF is most commonly used include:
Blocked or damaged fallopian tubes: If both tubes are blocked, sperm cannot reach the egg naturally. IVF bypasses the tubes entirely by fertilizing outside the body.
Male factor infertility: Low sperm count, poor motility, abnormal morphology, or azoospermia (no sperm in the ejaculate). IVF combined with ICSI allows fertilization even with very severe sperm problems. For men with no sperm in the ejaculate, TESA or TESE procedures can retrieve sperm directly from the testicle for use in ICSI.
Endometriosi:. The presence of endometrial tissue outside the uterus damages reproductive organs and reduces fertility. IVF offers better outcomes than natural conception attempts for women with moderate to severe endometriosis.
PCOS (Polycystic Ovary Syndrome): When ovulation induction and IUI have not resulted in pregnancy, IVF becomes the appropriate next step. With careful protocol management, women with PCOS can achieve good outcomes from IVF.
Ovulation disorders and premature ovarian insufficiency: When ovaries do not produce eggs regularly or at all, IVF using the woman’s remaining eggs or donor eggs is the available pathway.
Unexplained infertility: When both partners’ individual test results appear normal but pregnancy has not occurred after a year or more of trying, IVF offers the best chance of success by taking control of the fertilization environment.
Advanced maternal age: From the late 30s onward, egg quality and quantity decline. IVF, sometimes combined with preimplantation genetic testing, or using donor eggs, gives older couples a medically managed pathway to parenthood.
Genetic conditions: Preimplantation Genetic Testing (PGT) can be performed on embryos before transfer to screen for chromosomal abnormalities or specific inherited disorders, reducing the risk of passing serious genetic conditions to the child.
Explore our complete guide, “How Fertility Clinics Monitor Ovulation and Follicle Growth,” to better understand fertility tracking and treatment success.
The History of IVF in Nepal
Nepal entered the world of IVF much later than Western countries, but the growth since then has been remarkable.
Om Hospital and Research Centre in Kathmandu opened its first IVF facility in 2004. On 3 March 2005, Om Mani Tamang was born as Nepal’s first IVF baby, the child of Rajendra and Sandhya Tamang, who had faced multiple miscarriages and tubal infertility. The birth was celebrated widely, confirming that world-class assisted reproduction was now possible within Nepal.
Up to 2015, only four or five centers were providing IVF services in the country. As awareness grew and more couples recognized that they no longer needed to travel to India for treatment, the sector expanded rapidly. According to the Kathmandu Post, the Fertility Society of Nepal (FESON) estimated around 30 IVF clinics had gained registration from the Ministry of Health, with services increasingly available in cities beyond Kathmandu.
Critically, with the introduction of IVF services in Nepal, an estimated 70% of Nepali couples who had previously needed to travel to India for fertility treatment were able to access care domestically, saving significant time, money, and the added stress of managing treatment in a foreign city.
Today, Nepal offers not just basic IVF but the full range of advanced fertility techniques: ICSI for male infertility, frozen embryo transfer, donor sperm and egg programs, preimplantation genetic testing, and comprehensive fertility preservation. Clinics like Sishu Fertility Clinic, with locations in Chitwan and Dang, have brought specialist fertility care to couples in central and western Nepal who previously had no viable local option.
Why IVF Is Particularly Important in Nepal
Understanding why IVF matters specifically in Nepal requires understanding what infertility means in this country, not just medically, but socially.
Infertility Is Common and Underacknowledged
The World Health Organization estimates that roughly 1 in 6 people of reproductive age globally experience infertility at some point in their lives, representing approximately 17.5% of the adult population. This figure holds consistently across income levels, meaning Nepal is not exempt from a global pattern that affects hundreds of millions of people. FESON’s own estimates place the proportion of infertile couples in Nepal at approximately 15 to 20%, with around 15% of those cases requiring IVF-level intervention.
These are not small numbers. They represent a substantial proportion of married couples across the country, many of whom are silently managing a medical condition that has been mislabeled as a personal failing or a spiritual punishment.
The Cultural Burden Falls Disproportionately on Women
Research published in the Journal of Balkumari College in 2025, based on case studies from Bharatpur, found that when pregnancy is delayed, Nepali society is quick to assign blame to the woman, rarely to the man. Couples in both urban and rural areas of Bharatpur reported significant mental, domestic, and social stress related to their infertility. In rural communities, some couples still attributed infertility to the anger of ancestors or gods, turning to traditional healing before seeking medical evaluation.
Published research on infertility in developing countries more broadly confirms this pattern: in societies where childlessness carries severe stigma, women are frequently blamed, isolated, and in some cases subjected to domestic pressure or marital instability as a consequence of infertility that is often not their own.
The reality, established by decades of global research, is that male factors contribute to infertility in roughly 40 to 50% of all cases. When both partners are evaluated together from the start, as good clinical practice requires, many couples discover that the cause of their infertility lies with the male partner or with both partners simultaneously. IVF, and ICSI in particular, treats infertility as a couple’s medical condition rather than a woman’s failure.
IVF Breaks the Barrier of Structural Infertility
Many Nepali women experience blocked fallopian tubes from untreated pelvic infections, post-surgical adhesions, or prior ectopic pregnancies. For these women, fertility medications and IUI cannot work because there is no physical pathway for sperm to reach the egg. IVF is the only viable treatment. It bypasses the blockage entirely by retrieving eggs directly from the ovary and fertilizing them in the laboratory.
The same applies to women with endometriosis severe enough to compromise natural conception, and to men with zero sperm in the ejaculate where surgical sperm retrieval combined with ICSI represents the only path to biological fatherhood.
Nepali Couples No Longer Need to Travel Abroad
Before IVF was available in Nepal, couples who could afford treatment had to travel to India, usually Kolkata, Delhi, or Bangalore, bearing not only the cost of the procedure but the cost of transport, accommodation, time away from work, and the emotional difficulty of managing a medically and emotionally demanding process far from home and family.
The growth of quality fertility clinics within Nepal has changed this fundamentally. Access is no longer exclusively a Kathmandu story either. Clinics in Chitwan and Dang now serve couples from across the Terai and the western hills, meaning that specialist fertility care is increasingly accessible outside the capital.
Affordability Relative to the Region
IVF in Nepal is meaningfully more affordable than in India’s major cities or Western countries, while drawing on comparable technology and expertise. A standard IVF cycle in Nepal costs approximately NPR 2,50,000 to NPR 5,00,000 depending on the clinic, the medications needed, and whether additional procedures such as ICSI or frozen embryo transfer are required. This remains a significant sum for many Nepali households, and the absence of any government insurance or public subsidy for fertility treatment is a genuine barrier. But it is considerably lower than the equivalent cost in India, Thailand, or any Western country, making Nepal the most accessible regional option for couples in the country.
What IVF Can and Cannot Do

IVF is powerful and genuinely life-changing for many couples. It is also worth being clear about its limits.
IVF cannot reverse the biological decline in egg quality that comes with age. It cannot guarantee a pregnancy from any given cycle. It cannot make a chromosomally abnormal embryo into a healthy one. The success of any IVF cycle depends on the woman’s age, ovarian reserve, the specific cause of infertility, embryo quality, and the experience of the clinical and embryology team performing the procedure.
For women under 35, success rates per cycle using their own eggs are generally in the 40 to 50% range at experienced clinics. These rates decline progressively with age, and by the early 40s, success per cycle with own eggs is substantially lower. Multiple cycles are often needed before a successful pregnancy is achieved.
These are not reasons to avoid IVF. They are reasons to approach it with accurate information, with realistic expectations, and with a medical team that is honest with you about where you stand and what your options are.
Frequently Asked Questions
What does IVF stand for?
IVF stands for In Vitro Fertilization. “In vitro” means outside the body in Latin. The procedure involves fertilizing an egg with sperm in a laboratory rather than inside the woman’s body, and then transferring the resulting embryo into the uterus.
Who was Nepal’s first IVF baby?
Nepal’s first IVF baby was Om Mani Tamang, born on 3 March 2005 at Om Hospital and Research Centre in Kathmandu. His parents, Rajendra and Sandhya Tamang, had experienced multiple miscarriages and tubal infertility. His birth marked the beginning of IVF services in Nepal.
How long does one IVF cycle take?
A complete IVF cycle from the start of ovarian stimulation to the pregnancy test takes approximately four to six weeks. The stimulation phase alone lasts 8 to 14 days. After embryo transfer, the two-week wait period follows before a pregnancy blood test can give a reliable result.
Is IVF the same as ICSI?
No, but they are closely related. IVF is the broader process that includes egg retrieval, fertilization, embryo culture, and transfer. ICSI is a specific fertilization method used within IVF, where a single sperm is injected directly into the egg rather than allowing sperm to fertilize naturally in a dish. ICSI is recommended when there is significant male infertility.
Is IVF painful?
The egg retrieval procedure is done under sedation and is not experienced as painful during the procedure. Mild cramping and discomfort in the day or two afterward are common. The injection phase can cause bloating and physical discomfort as the ovaries enlarge. Embryo transfer is generally painless and requires no anesthesia.
How much does IVF cost in Nepal?
A standard IVF cycle in Nepal typically costs between NPR 2,50,000 and NPR 5,00,000. The total depends on the medications needed, whether ICSI or other additional procedures are required, and the specific clinic. Our IVF Cost in Nepal page provides a more detailed breakdown.
Is IVF available outside Kathmandu in Nepal?
Yes. Sishu Fertility Clinic offers full IVF services at locations in Chitwan (CMS Road, Bharatpur) and Dang (BP Chowk, Ghorahi), making specialist fertility care accessible to couples in central and western Nepal without the need to travel to Kathmandu.
What is the success rate of IVF in Nepal?
Success rates in Nepal, as everywhere, vary based on age, diagnosis, and clinic. For women under 35 with good ovarian reserve, success rates per cycle are generally in the 40 to 50% range. Rates decline with age and are lower when there are additional complicating factors. Your treating specialist will give you a more personalized estimate based on your own assessment results.
Does IVF guarantee a pregnancy?
No. IVF is the most effective fertility treatment available, but it does not guarantee pregnancy from any single cycle. Many couples achieve pregnancy within one or two cycles. Others need more. Success depends on egg quality, sperm quality, embryo development, uterine receptivity, and the specific cause of infertility. Accurate information and realistic expectations matter as much as the medical treatment itself.