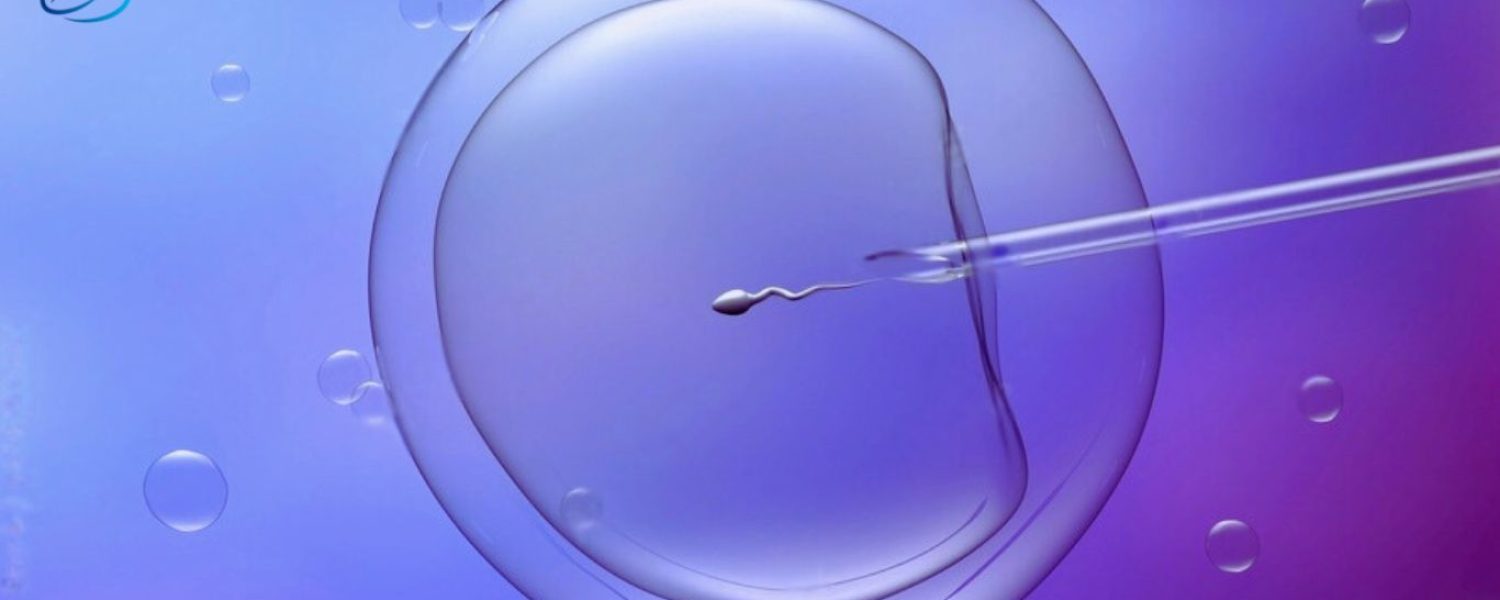
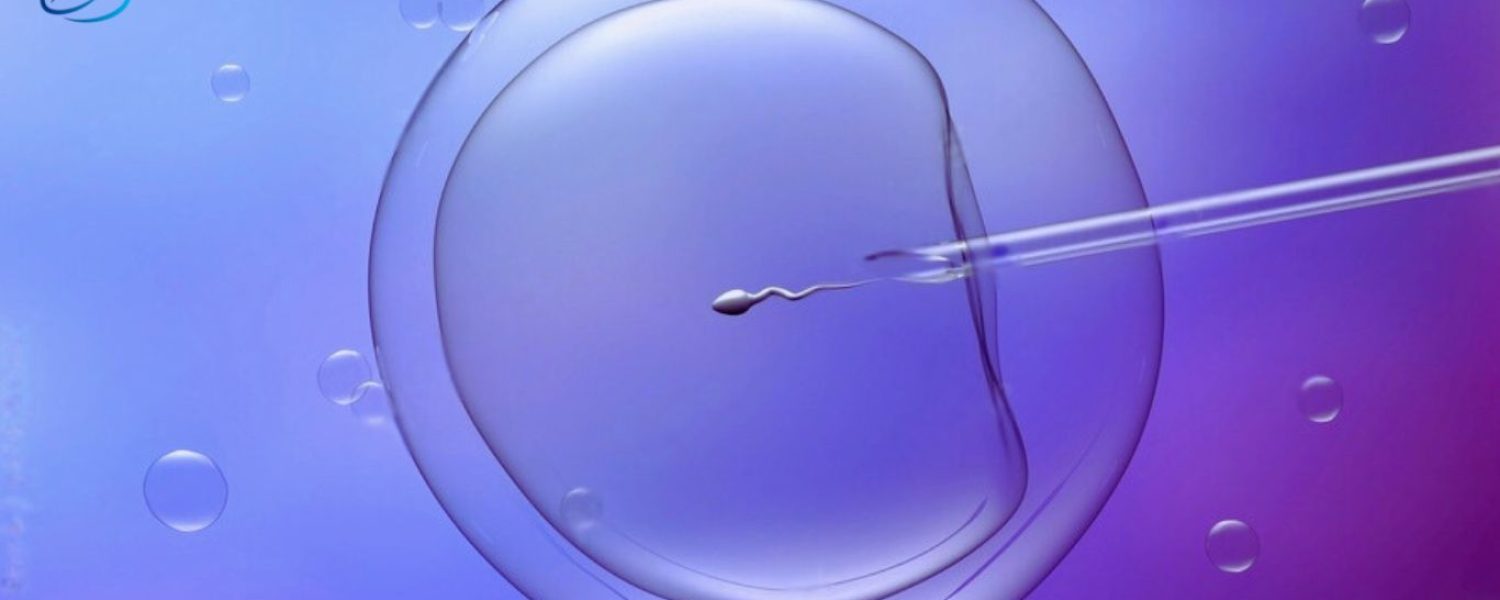
Intracytoplasmic Sperm Injection (ICSI) is an advanced fertility treatment where an embryologist takes a live sperm and injects sperm directly into an egg (cytoplasm of an egg). ICSI is used when there are severe male infertility issues or previous IVF attempts have failed.
Difference Between ICSI and In Vitro Fertilization(IVF)
In IVF, eggs are retrieved from the woman’s ovaries and combined with sperm in vitro (test tube), and fertilization occurs naturally.
But During ICSI, a selected single sperm is directly injected into the cytoplasm of the retrieved egg using a fine needle.
Use Cases Difference
IVF: IVF is used for various fertility issues, including unexplained infertility, blocked fallopian tubes, endometriosis, and male factor infertility.
ICSI: ICSI is specifically employed when male partners have low sperm count, poor sperm motility, or difficulty penetrating the egg.
Success Rates Difference
IVF: IVF success rates vary, but it fertilizes around 70% to 80% of eggs.
ICSI: ICSI has a higher fertilization rate (75% to 85%) due to the direct injection method.
Cost Difference
IVF: IVF is less complex and often less expensive than ICSI.
ICSI: ICSI involves additional steps and costs more due to the intricate sperm injection process.
Features | ICSI (Intracytoplasmic Sperm Injection) | IVF (In Vitro Fertilization) |
Fertilization Method | A single selected sperm is injected directly into the cytoplasm of the egg. | Sperm and eggs are mixed in a dish, allowing natural fertilization. |
Use case | Low sperm count, poor sperm motility, difficulty with sperm penetrating the egg. | Unexplained infertility, blocked fallopian tubes, endometriosis, mild male factor infertility. |
Success rate (in Nepal) | 75% – 85% (higher due to direct injection) | 70% – 80% |
Cost | More complex and often more expensive due to the sperm injection process. | Less complex and often less expensive. |
Process of ICSI
Intracytoplasmic Sperm Injection (ICSI) is a specialized fertility treatment used during in vitro fertilization (IVF).
- Egg Retrieval: The woman undergoes ovarian stimulation to produce multiple eggs and a minor surgical process is carried out for Oocyte retrieval.
- Sperm Collection: The male partner provides a semen sample. If there are sperm-related issues (ejaculation issues or poor motility), a urologist may extract sperm directly from the testicles or epididymis.
- Sperm Selection: Under a high-powered microscope, an embryologist selects a healthy sperm for injection. ICSI is particularly useful when sperm quality is compromised.
- Microinjection: With a fine glass needle, the selected sperm is injected directly into the egg’s cytoplasm for fertilization.
- Embryo Culture: The fertilized egg (now an embryo) is cultured in the lab for a few days. It undergoes cell division and development.
- Embryo Transfer: One or more viable embryos are transferred into the woman’s uterus after Preimplantation Genetic Testing (PGT) test is done.
ICSI is beneficial for severe male infertility cases and can improve fertilization rates. It is essential to discuss risks and success rates with a fertility specialist if you have fertility issues.
How long does an ICSI cycle take?
The Intracytoplasmic Sperm Injection (ICSI) cycle typically lasts 2-3 weeks.
- Ovarian Stimulation: About 10-12 days. The woman receives hormonal injections to stimulate egg production.
- Egg Retrieval: A minor surgical procedure lasting 20-30 minutes.
- Sperm Collection and Selection: A few hours. The embryologist selects a healthy sperm.
- Microinjection (ICSI): Takes minutes per egg.
- Embryo Culture: Embryos develop in the Incubators for 3-5 days.
- Embryo Transfer: A brief procedure.
What are the risks of ICSI?
ICSI is safe and effective for couples with male-factor infertility cases. It increases the chances of fertilization in such cases.
However, ICSI has some risks associated with it.
- Increased risk of miscarriage.
- Heart and brain problems in infants that may require surgery.
- Increased risk of Social interaction and communication difficulties.
- Increased risk of delayed speech, learning difficulties, and mood disorders.
- Risk of Multiple Pregnancy.
Additionally, some studies suggest that ICSI may be associated with an increased risk of chromosomal abnormalities, autism, intellectual disabilities, and birth defects compared to conventional IVF.
What are the success rates of ICSI?
The success rate of ICSI(Intracytoplasmic Sperm Injection) is 70-80%.
The subsequent IVF treatment and successful embryo implantation play a crucial role in achieving a live birth.
Keep in mind that no procedure can guarantee a 100% success rate.
What factors affect ICSI success rates?
Several factors (like age, embryo, and sperm quality) affect the success rates of Intracytoplasmic Sperm Injection (ICSI)
- Female Age: Younger women tend to have better outcomes. Fertility declines with age.
- Quality of Embryos: High-quality embryos have a higher chance of implantation.
- Sperm Quality: ICSI is often used for male factor infertility. Better sperm quality improves success rates.
- Underlying Conditions: Conditions like endometriosis or polycystic ovary syndrome (PCOS) impact success.
- IVF Clinic Expertise: Experienced clinics tend to achieve better results.
How many embryos are transferred during ICSI?
The standard practice for ICSI is to transfer one embryo (occasionally two) at a time. This approach minimizes the chance of multiples while maintaining similar cumulative live birth rates per IVF cycle.