Male Infertility Treatment in Nepal
Facing male infertility can be challenging, but you’re not alone. At Sishu Fertility Clinic, we provide compassionate support, accurate diagnosis, and advanced treatment options tailored to your needs. From identifying underlying causes to offering proven solutions like IVF and ICSI, our expert team is here to guide you every step of the way, helping you improve your chances of starting a healthy, happy family.
WHAT IS MALE INFERTILITY?
Male infertility is the inability of a male to impregnate a woman even after a year of unprotected sexual intercourse. A male is entirely responsible for around 20% of infertility cases and is a contributing factor in another 30% to 40% of all infertility cases. Mostly, the male and female cases co-exist, hence it is crucial that both the partners are investigated for infertility and managed together. Moreover, the male factor substantially contributes to around 50% of all cases of infertility.
There is a heap of reasons why male infertility occurs, including both reversible as well as irreversible conditions. Other factors that might influence each of the partners could be their age, medications, exposure to environmental toxins, genetic problems, and systematic diseases.

Why Choose Sishu Fertility Clinic for MALE INFERTILITY Treatment in Nepal?
At Sishu Fertility Clinic, we understand the profound desire to build a family. That’s why we’re dedicated to providing the highest quality IVF treatment in Nepal to help you achieve your dream of parenthood. Here’s what sets us apart:
Sishu Fertility Clinic has consistently high IVF success rates.
Our team includes the most experienced fertility specialists, embryologists, and nurses.
Our team includes the most experienced fertility specialists, embryologists, and nurses.
We utilize advanced technology and the latest techniques in reproductive medicine, including advanced embryo culture systems, Preimplantation Genetic Testing (PGT), and time-lapse embryo monitoring.
Every patient is unique, and so are our treatment plans. We understand your circumstances and develop a customized IVF plan to maximize your success rate.
We prioritize clear and honest communication that includes the costs, potential risks, and expected outcomes before IVF.
Male Infertility Causes
Azoospermia: No sperm cells in the semen because of any physical obstructions, hormonal issues, or testicular failure could be the reason behind infertility.
Oligospermia: Low sperm count or poor sperm motility can also lead to decreased chances of fertilization.
Genetic Disorder: Another cause might be a genetic disorder like Klinefelter syndrome, Y chromosome microdeletions, and cystic fibrosis that can affect sperm quality as well as production.
Hormonal issues: Hormonal imbalance issues like low testosterone levels or high prolactin levels can also impact sperm function and production.
Varicocele: Enlarged veins in the scrotum, which can cause heat damage to the sperm and, in turn, affect the sperm count and motility.
Infection: Infections like prostatitis, epididymitis, and sexually transmitted infections, can also damage the sperm as well as the reproductive organs.
Medications and drugs: Some medications like anabolic steroids, chemotherapy, or recreational drugs can also impact sperm production and function.
Environmental factors: High exposure to toxins, radiation, or excessive heat (from saunas or even laptops) can damage the sperm.
Lifestyle factors: Your day-to-day lifestyle factors might also lead to male infertility, such as smoking, alcohol consumption, and a poor diet. These things will affect your overall health and, in turn, sperm production.
Age-related infertility: Sperm count as well as the quality of sperm tends to decline as men age.
Erectile dysfunction and Ejaculation disorders: These disorders can affect a man’s ability to achieve or maintain an erection or to ejaculate properly.
Trauma to the testes: This can damage the reproductive organs and severely affect sperm production and function.
There might be several other possible causes behind the male infertility issue. A doctor or fertility specialist will be able to identify the potential causes and create a treatment plan accordingly.
Considering IVF in Nepal?
Don’t hesitate to reach out to Sishu Fertility Clinic today. Schedule a consultation with our fertility specialists to discuss your unique situation and explore how IVF can help you achieve your dream of parenthood.
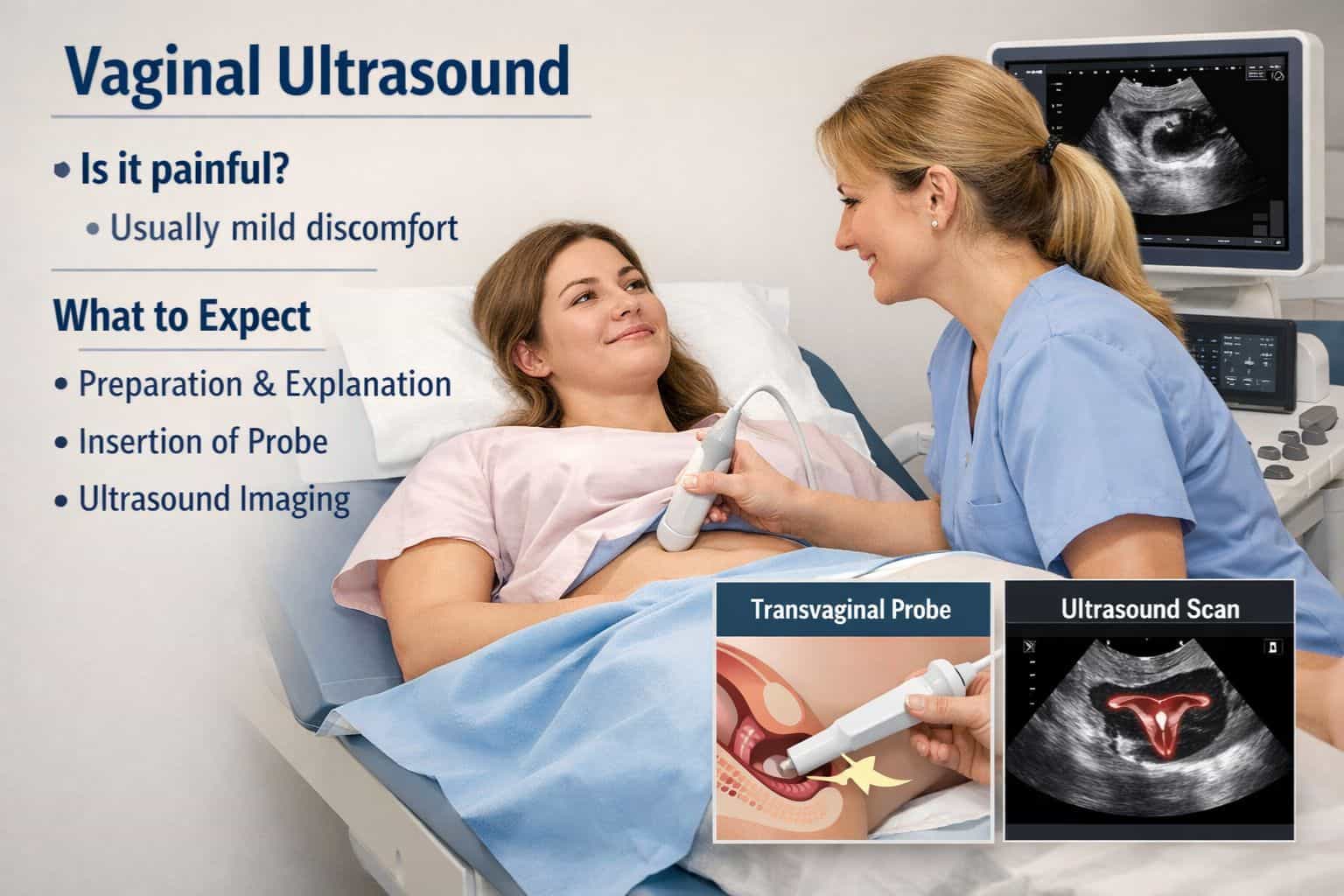
LEARN ABOUT TESTING AND DIAGNOSIS
Once a new semen sample is collected either through self-stimulation at home or at the Sishu Fertility Clinic collection location, our laboratory team will closely examine it under a microscope to analyze the following component:
VOLUME
Semen volume is the amount of ejaculated fluid. Usually, the semen volume falls between 1.5 to 5 milliliters. Lower semen volumes lead to a low sperm count and are associated with a reduced fertility rate. Normal semen contains at least 15 million sperm per milliliter. There are a lot of reasons affecting semen volumes including psychological issues.
MOTILITY
The term sperm motility refers to the movement of a man’s sperm. The analysis assesses if the sperm are swimming properly and are in a straight line. Then, the sperms receive letter grades starting from A to D, A being the fastest and straightest swimmers, and a D is given to those that don’t move at all. If the test sample reveals that less than 25 to 30 percent of the sperm are moving forward progressively then the sperm motility is regarded as low.
MORPHOLOGY
Sperm morphology refers to the shape of the sperm, which includes head size and head DNA content (revealed by a nuclear color stain), the midpiece appearance, and the structure of the tail. The head shape plays an important role as it can affect the sperm’s ability to penetrate the outer surface of a woman’s egg to fertilize it.
CONCENTRATION
The concentration of sperm or sperm density is the total number of sperm per milliliter of semen. Sperm concentration is regarded as an important influence on fertility. According to the world health organization(WHO), normal sperm concentration ranges anywhere from 15-259 million sperm per milliliter.
APPEARANCE
Appearance of the semen can indicate any unlying issues. Normal semen is usually a whitish-gray color, and might have a slightly yellowish tint. The consistency of semen is typically thick and viscous but becomes more liquid after ejaculation.
When the appearance of semen is abnormal in terms of clarity, color, or consistency, this might be an indication of any underlying issue. If semen is yellowish or greenish in color then it may indicate the presence of infection and if it is reddish-brown then it may indicate the presence of blood.
MALE HORMONE TESTING
We may, from time to time, conduct a blood test to check for genetic or hormonal conditions. These causes are generally less prevalent than others. As a result, testing is rarely carried out unless there are additional underlying factors.
We rely on extensive fertility testing and analysis at Shisu Fertility Clinic.
There are a lot of treatment options that we might suggest if we discover a problem with the semen analysis that could make it hard to get pregnant. A consultation with a urologist, a specialist in male infertility, will be our recommendation.
MALE INFERTILITY TREATMENTS
IUI
IUI stands for intrauterine insemination. It’s also sometimes called donor insemination, alternative insemination, or artificial insemination. IUI works by putting sperm cells directly into your uterus around the time you’re ovulating, helping the sperm get closer to your egg. This cuts down on the time and distance sperm travels, making it easier to fertilize your egg.
IVF
IVF stands for In virto fertilization. This is a type of assisted reproductive technology that includes the fertilization of an egg with the sperm outside of the female body, in a laboratory dish or test tube. This process starts with the stimulation of the ovaries to produce multiple eggs. After that, these eggs are retrieved and mixed with sperm in a laboratory dish for fertilization.
ICSI
ICSI (Intracytoplasmic Sperm Injection) is a form of assisted reproductive technology used to treat male infertility. In traditional IVF (In vitro fertilization), the sperm is introduced to the egg in a dish and left to fertilize naturally. However, in cases where the sperm is not able to penetrate the egg due to low motility or abnormal morphology, ICSI can be used to directly inject a single sperm into the egg to facilitate fertilization.
VARICOCELE SURGERY
Because a varicocele rarely produces symptoms, it is not uncommon for a man not to be aware of it unless it causes problems with fertility. Surgical treatment redirects the blood flow toward normal veins. Surgery is done on an outpatient basis.
PESA
Percutaneous Epididymal Sperm Aspiration (PESA) is a procedure that involves a fine needle being passed into the epididymis for fluid extraction which is then checked immediately by the embryologist for the presence of sperm. The epididymis is a duct that is behind the testes where sperm cells are collected and mature prior to ejaculation.
MESA
Microsurgical Epididymal Sperm(MESA) refers to the retrieval of sperm-containing fluid from the epididymis that is sent for processing and extraction of the sperms. This procedure is conducted using an operating microscope that provides the high optical magnification required for this procedure. To induce fertilization and pregnancy, the extracted sperm is then directly injected into the partner’s egg by a procedure known as Intracytoplasmic sperm injection or ICSI.
TESE
TESE(Testicular Sperm Extraction), is the extraction of small portions of the tissue from the testicle through a minor surgical procedure under anesthesia. This procedure is also referred to as testicular biopsy. After the treatment of the tissue samples, usually, it is possible to extract single sperm cells that can later be used for fertility treatments like ICSI.
FAQs About MALE INFERTILITY TREATMENTS in Nepal
1. What is male infertility?
Male infertility is the inability of a male to impregnate a woman even after a year of unprotected sexual intercourse. Males are entirely responsible for around 20% of infertility cases and contribute to another 30–40% of all cases. Since male and female infertility often co-exist, it is important that both partners are investigated and managed together.
2. What are the most common causes of male infertility?
There are several causes of male infertility including azoospermia (no sperm in semen), oligospermia (low sperm count or poor motility), hormonal imbalances like low testosterone or high prolactin, varicocele (enlarged veins in the scrotum), genetic disorders such as Klinefelter syndrome, infections like prostatitis or STIs, certain medications, environmental toxin exposure, lifestyle factors.
3. How is male infertility diagnosed at Sishu Fertility Clinic?
Diagnosis begins with a semen analysis, where a fresh sample is examined under a microscope. The lab team evaluates five key parameters: semen volume, sperm motility (movement), sperm morphology (shape), sperm concentration (count per milliliter), and semen appearance (color and consistency). In some cases, a hormone blood test may also be conducted to check for genetic or hormonal conditions.
4. What does sperm motility mean and why does it matter?
Sperm motility refers to the movement of sperm. During semen analysis, sperm are graded from A to D based on their swimming speed and direction — A being the fastest and straightest, D being completely immobile. If less than 25–30% of sperm are moving forward progressively, motility is considered low, which reduces the chances of natural fertilization.
5. What is a normal sperm concentration according to WHO?
According to the World Health Organization (WHO), normal sperm concentration ranges from 15 to 259 million sperm per milliliter of semen. Normal semen should contain at least 15 million sperm per milliliter. A count below this threshold is associated with reduced fertility.
6. What male infertility treatments are available at Sishu Fertility Clinic?
Sishu Fertility Clinic offers a range of male infertility treatments depending on the diagnosis. These include IUI (intrauterine insemination), IVF (in vitro fertilization), ICSI (intracytoplasmic sperm injection), varicocele surgery, PESA (percutaneous epididymal sperm aspiration), MESA (microsurgical epididymal sperm aspiration), and TESE (testicular sperm extraction).
7. What is ICSI and when is it used for male infertility?
ICSI (Intracytoplasmic Sperm Injection) is a specialized form of assisted reproductive technology used when sperm cannot naturally penetrate the egg due to low motility or abnormal morphology. Unlike traditional IVF, where sperm and egg are left to fertilize naturally in a dish, ICSI involves directly injecting a single sperm into the egg to facilitate fertilization.
8. What is TESE and how does it help with male infertility?
TESE (Testicular Sperm Extraction) is a minor surgical procedure performed under anesthesia where small portions of tissue are extracted from the testicle, also referred to as a testicular biopsy. After processing the tissue samples, individual sperm cells are extracted and can be used in fertility treatments like ICSI to achieve fertilization and pregnancy.
9. What is varicocele and how is it treated?
A varicocele is the enlargement of veins in the scrotum, which can cause heat damage to sperm and negatively affect sperm count and motility. Because it rarely produces symptoms, many men are unaware of it until it causes fertility issues. It is treated through surgery, which redirects blood flow toward normal veins. The procedure is performed on an outpatient basis.
10. Why choose Sishu Fertility Clinic for male infertility treatment in Nepal?
Sishu Fertility Clinic stands out for its experienced team of fertility specialists, embryologists, and nurses, along with consistently high IVF success rates. The clinic uses advanced technology including Preimplantation Genetic Testing (PGT) and time-lapse embryo monitoring. Every patient receives a customized treatment plan, and the clinic maintains transparent communication about costs, risks, and expected outcomes.
Latest Information Blogs
Find out the latest blogs about our Sishu Fertility Clinic & IVF center and information about all your fertility and health-related needs. We are always happy to hear what you have to say so be sure to leave a comment.